Mali posts modest gains in child health
Mali posts modest gains in child health
Mali remains among the most dangerous places on earth to be an infant or child, despite clear improvements in the past decade. Nearly one child in four will die before the age of five. One in three suffers chronic malnutrition.
The picture is typical of West Africa's Sahel region as a whole. In part, it reflects the state of Mali's lamentable health care system. In the late 1990s only 30 per cent of the population had access to even rudimentary health services -- in Africa, only Benin and the Democratic Republic of Congo were worse off. Barely half the population had access to clean water.

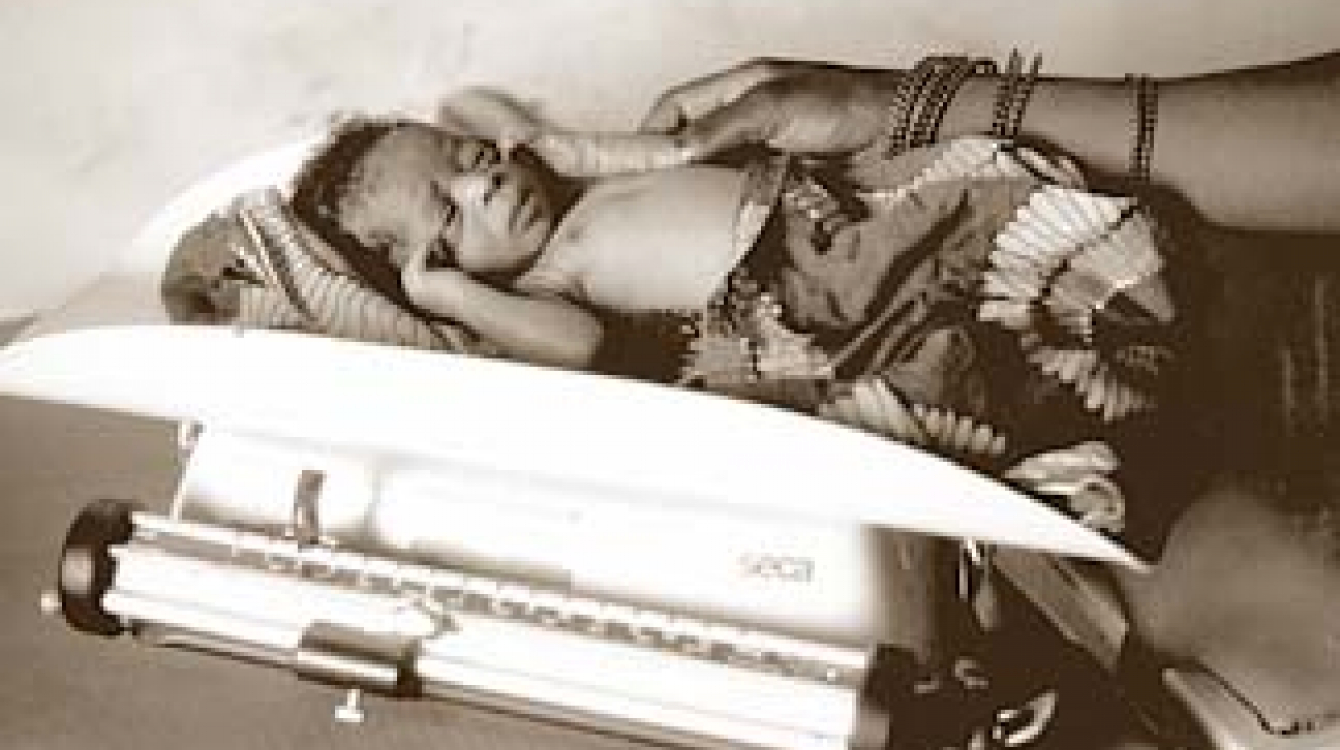
An infant being weighed at a community clinic in Dougouolo, Mali: there have been some improvements in child health over the past decade.
Photo : ©UNICEF / Giacomo Pirozzi
Yet some of these statistics were considerably worse in the 1980s. Although the figures remain among the world's grimmest, there have been some gains. One success in the 1990s was the complete elimination of polio. The incidence among infants, always high in Mali, had rocketed in the 1970s and 1980s. But the launch of an extensive vaccination campaign in 1988 was one of Mali's earliest child health successes: the last case of polio was recorded in 1995. There have been other advances. Guinea worm has been effectively eradicated. Yellow fever is absent for now. Hansen's Disease (leprosy) is increasingly a thing of the past. River blindness is said to be in steep decline.
Yet comprehensive vaccinations for polio and "DPT3" (diphtheria, pertussis and tetanus) still cover only 52 per cent of children. The worst killers -- malaria and dysentery -- remain rife. Nevertheless, life expectancy at birth may now be as high as 55 years, up from a mere 46 years in 1990, according to the UN Development Programme.
The improvements of the past decade are due to a combination of factors, many of them influenced by the changed political situation. The government has consciously shifted spending from the military to health and other social sectors since the end of President Moussa Traoré's dictatorship in 1991. The gradual entrenchment of democratic institutions, decentralization of administrative services, improved accountability, a vigilant independent media and the maintenance of peace since the end of the Tuareg rebellion in 1996 have all permitted some continuity in policy and made it possible to deliver health care to many Malians who previously received none.
Devaluation and adjustment
Although conscious policy decisions have been an important factor in the improvements, the wider economic situation has also influenced the short-term picture, and not always in a positive direction. The key event of the past decade was the 50 per cent devaluation in 1994 of the CFA franc, which Mali shares with 13 other countries, most of them former French colonies. The results have been mixed.
The evidence suggests that family and child welfare in rural areas benefited from shifts in the domestic terms of trade in favour of the countryside, that is, an increase in villagers' relative incomes, compared with the prices they had to pay for basic consumer goods. This was one of the main goals of the devaluation. It was reinforced by a lucky combination of good harvests, revamped food security mechanisms, sharply expanded cotton production at a time of revived world prices -- boosting incomes in the cotton-growing rural south especially -- and the expansion of medical outreach and village pharmacy initiatives after 1994.
There have been exceptions, however. In addition to the far north, isolated zones such as the Bankass and Tominian areas, near the border with Burkina Faso, see unusually high levels of infant illness and malnutrition. The causes are complex, but include closely spaced pregnancies, which have reduced breastfeeding periods per child, affecting infant nutrition. Poor soil and drought mean an unusually poor diet.
Decentralization on its own is no guarantee of improved basic health provision for children. However, the Malian experiment may be among Africa's most credible.
Mali's urban population bore the full brunt of the devaluation. Because they were more exposed to the wider world economy, townsfolk were hit more directly than villagers by the higher costs of imports. This blow came on top of the rigours of Mali's structural adjustment programme, initiated in the late 1980s under pressure from the International Monetary Fund (IMF). The earlier phases of that programme paid no attention to social priorities, and the government was sluggish in addressing the scandalous provision and price of medicines as basic as infant rehydration compounds. Tellingly, key targets of rioters at the height of the 1991 "revolution" against President Traoré included the hated state pharmacies.
Bamako, the capital, is now home to at least one Malian in 10. Its urban economy has been transformed in the past decade, and a new middle class is emerging. But health services in poor outer suburbs such as Sénou and Sebenikoro remain minimal. Embryonic water and sewage systems have deteriorated because of excessive use. Living costs keep rising, and children inevitably bear the brunt of absolute poverty. In Bamako's worst shantytowns, it is survival of the fittest.
Five-year health programme
A key element in Mali's ability to make some progress despite the difficult economic circumstances has been its five-year health investment plan, known as the Programme de développement sanitaire et social (PRODESS). Launched in 1998, it is coordinated with a range of other social and economic plans.
PRODESS was the result of an unprecedented two-year process of consultations with all stakeholders, above all local communities and women. It was also realistically budgeted, something that was rarely true under previous health initiatives. Its main elements include:
- increased nationwide basic health coverage, through 347 centres specializing in speedy health care
- improved outreach services for "peripheral" areas, including low-population zones, with a growing emphasis on preventative medicine
- the establishment of a Federation of Community Health Associations, building on the extraordinary growth in community associations in the 1990s
- a nationwide system for supplying basic medicines.
PRODESS has as its motto "Health for All," but there is no doubt that infants and small children will benefit most from this level of health coverage. Its stress on equitable standards and geographical distribution of health centres is a departure from previous approaches. So is the idea of community ownership.
An initiative by the French Médécins du monde (MDM) in Mali's vast north, at the desert's edge, illustrates how the PRODESS plan relies on better coordination with non-governmental organizations (NGOs). Goundam, in the region of Timbuktu, has a population of 150,000, including 30,000 returned refugees from the 1990-96 conflict between the army and Tuareg rebels. This semi-nomadic population covers an immense territory and is among the country's very poorest. Levels of maternal and infant mortality unsurprisingly reflect this. Since 1996, the MDM has opened 13 bush clinics situated on migratory routes, with the express aim of reducing miscarriages and new-born deaths, as well as mother and infant malnutrition.
Another example of NGO action tailored to PRODESS's overall plan is a medicine project of Pharmaciens sans frontières (PSF), also from France, in the Sikasso region. Close to the southern border with Côte d'Ivoire, the densely populated area has been surprisingly poorly served since independence, especially where child health is concerned. The main aim of the PSF's five-year project is to boost access to reasonably priced medicine from 20 per cent of the local population to 80 per cent, with special emphasis on rural women and children.
Decentralization
The government's decentralization programme is another factor that may improve children's fortunes over the medium-term. Developed gradually between 1993 and 2000, it aims to devolve both essential local services and the authority to fund them to 701 specially created communes (19 of them urban). Among these are basic health and education. This is a radical departure from the highly centralized state system bequeathed to Mali at the time of its independence from French colonial rule in 1960. Despite the centralization of official government bodies, informal local decision-making mechanisms have survived surprisingly well, especially at village level, and the new initiative seeks to build on this.
As with PRODESS, it is too early to tell whether a corner has been definitively turned. Decentralization on its own is no guarantee of improved basic health provision for children, or of anything else. However, the Malian experiment may be among Africa's most credible. During the 1999 elections that finally brought the new system into being, women were targeted by the administration, NGOs and some political parties, with the message that voting was an effective way of ensuring that their and their children's interests would be taken into account. Radical feminism might face considerable resistance in the villages, observed one outreach worker, "but the men cannot object to improving the lot of their children."
Meanwhile, information circulates much more widely at the local level, thanks to an explosion of community radio stations broadcasting in Mali's indigenous languages. The independent media is often quick to criticize regional officials who try to abuse their positions. An evolving culture of representation is obliging local decision-makers to be held accountable.
Political will
Ultimately, the past decade's progress is the result of political will, administrative reforms and rather a lot of luck. PRODESS, for all its imperfections, is the first credible health plan Mali has seen. Key ministries -- especially the Ministry of Women -- have been galvanized. Despite bitter and often justified criticism of other policies, the government of President Alpha Oumar Konaré has kept child health near the top of its priorities.
This has sometimes meant facing down IMF officials demanding sharp budget cuts at any cost. Mali's admission to the heavily indebted poor countries (HIPC) debt-relief initiative in late 2000 was a further sign that the IMF and World Bank are trying to modify their earlier heavy-handed approach to one of Africa's most fragile economies.
Malian policymakers see HIPC as just a start. The debt burden is still unsustainable and adequate increases in future social spending depend upon a near-complete write-off of external debt. The country's interim Poverty Reduction Strategy Paper, which outlines how HIPC debt relief will be spent on social needs, is considered to be one of the best-prepared and credible in francophone West Africa.
Yet nothing can be taken for granted, by the government or its external partners. Reaching the child health targets depends on an average 5 per cent annual economic growth rate until 2008. In 2001, Mali's gross domestic product did not grow at all, although the IMF and government project that it should rise to about 6 per cent in both 2002 and 2003. Such a volatile growth trajectory is mostly beyond the government's direct control, but it will determine just how much scope there actually is for exercising political will. Since the famine crisis of the early 1980s, Mali has "lost" two generations of its young. It cannot afford to lose another.